We want something different
Health care is driven by positive intent, yet its complexities create friction for patients, providers and payers. Multiple points of approvals and alignment between providers and payers, along with disconnected information systems, lead to challenges in the individual patient experience. And the payer, provider and patient are put into an unnecessary cycle of “iterate until we get it right.”

Dr. Smith
Dr. Smith wants to generate a predictable revenue stream and to enable quality care delivery for Joan.

Joan
Joan wants the best possible care and a better understanding of next steps and costs.

ABC Payer
ABC Payer wants claims and payment accuracy to enable optimal patient outcomes.
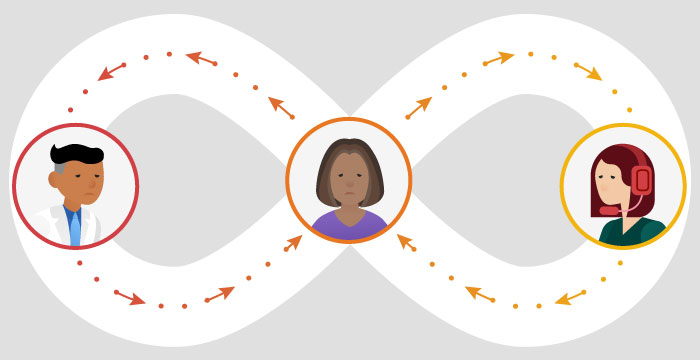
Joan is seeking care for a health issue. But getting care can be complex and she is caught in the middle between her doctor and her health plan. Joan’s clinical information is difficult for her doctor to access and use. Her doctor and her health plan need to align on multiple information requests and multiple approvals before Joan gets the care she needs. These delays are increasing Joan’s anxiety and worry.
The care experience is full of complexity for everyone
Dr. Smith's challenges:
- An incomplete view of evidence-based, next best actions for Joan
- Outdated clinical data for Joan
- An incomplete view of ABC Payer’s payment policies
- Unstable revenue stream
Joan's frustrations:
- Forced to referee between Dr. Smith and ABC Payer
- Anxiety and stress during an uncertain and scary time
- Costs for every interaction with Dr. Smith are complicated and unclear
- Uncertain of what to do next
ABC Payer's challenges:
- Incomplete clinical data for Joan
- Limited data-sharing and lag time
- Denials are time consuming and complex
- The most complete view of their own payment policy, which varies by payer
Our goal: Creating a transparent network where everyone wins
With solutions that foster next generation alignment between payers and providers — for the benefits of patients — we will reduce friction and waste, build greater collaboration and communication, and transform the underlying systems to better serve the people who rely on us.

Enable clinical/cost information sharing
- Proactively combine and share clinical and cost information for the payer, provider and patient.
- Share payer payment options upstream into provider claims workflows to validate claims based on payer agreements and required clinical data.

Eliminate lag time
- Drive the right, real-time clinical information to the point of care for more informed and clinically advanced patient decisions and improved care delivery.
- Eliminate prior authorization roadblocks between payers and providers.

Drive scalability
- Facilitate the provider-payer flow of clinical and cost information at scale to increase efficiency.
- Helps payers and providers to better partner on behalf of the patient.

Improve financial experience
- Modernize and streamline the financial side of health care using digital technology to deliver clear options and costs patients can navigate.
- Options are informed by evidence-based guidance and patient benefits and preferences.
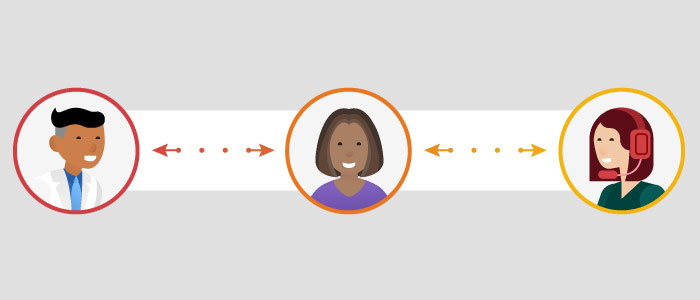
We see a connected and streamlined transparent network that simplifies the relationships between Joan, her doctor and her health plan. It is easier for Joan’s doctor to access and use her clinical information. Her health plan can share payment policies and claims editing rules with Joan’s doctor so claims are submitted correctly and approved. Joan now has peace of mind that her doctor and health plan have her best interest in mind. She better understands her care options, next steps and the costs.
A health care journey benefiting everyone
Dr. Smith’s experience now:
- Clinical and cost information are in sync
- Evidence-based medical standards are delivered at point of care
- Streamlined treatment approvals and payments are fully automated over time
Joan’s experience now:
- Clear and complete care plan
- Positive financial experience
ABC Payer’s experience now:
- Scales across the health care system
- Clarity of coverage in sync with Dr. Smith’s understanding


