What you should know about alternative funding
Alternative funding is a recent pharmacy benefits concept. A certain class of vendors promote alternative funding as a way for self-funded employers to make their employees and dependents eligible for “free” medications. Of course, the affected drugs are not free at all. Instead, these vendors arrange for funds to be diverted from vital funding sources like charitable organizations and foundations in order to reduce employer costs.
Here’s a summary:1
- Certain alternative funding vendors may try to convince plan sponsors to exclude some or all specialty drugs from their formulary to save money.
- Once the drugs are excluded from the plan, the member appears to be uninsured or underinsured. The alternative funding vendor can then help the “uninsured” patient apply for needs-based programs to cover the cost of the prescription intentionally removed from the plan’s coverage.
- When approved, the prescription is dispensed from a specific patient assistance program (PAP) pharmacy at no charge to the plan sponsor or patient.
Although this is how alternative funding programs are advertised to prospective clients, the reality can be much different. Unfortunately, alternative funding rarely works as advertised. It may introduce regulatory compliance risk and disrupt care for members.
The truth is that some alternative funding vendors are diverting charitable funds intended for people with little or no insurance coverage to those who actually are otherwise covered. In the process, they may charge fees ranging up to 25% of the cost of each drug.2
Needs-based funding for costly prescription drugs has an important role in the pharmaceutical market. But whether these funds come from manufacturer donations or private citizen contributions to charities, the charitable funding amount available is limited. Those who divert these funds to lower employer plan costs are effectively reducing the money available for people who need it most.
Growing popularity of alternative funding
Despite the drawbacks of alternative funding programs, employers are interested in the promise of lower costs. A recent survey found that up to 10% of self-insured plans with at least 5,000 employees were already using one of these programs. Another 27% said they were considering using one in the next 2 to 5 years.3
We think it’s time for a reality check. Let us explain why alternative funding isn’t a sustainable solution. In fact, it carries unexpected financial, clinical and even legal risks.
Financial risk
Health plans and employer groups are told that carving out parts of their pharmacy plan is simple and will save them money.4 It may be that adopting an alternative funding strategy is easy — at least at first. However, we believe that carving-out will likely have longer, unforeseen complications. Worse, it often causes patient treatment delays or disruptions.
We believe some alternative funding programs are making overstated, unsustainable promises. Plan sponsors seeking cost savings may not be considering the longer-term financial and regulatory risk of these strategies — both for themselves and the needs-based funding system overall.
As more employers use alternative funding, there are already signs that manufacturers and the charities they work with may stop providing funds to patients otherwise covered by insurance. In fact, it’s already happening in the marketplace. We’re hearing reports of patients receiving alternative funding having their eligibility removed due to new qualification criteria.
Alternative funding sources have always been limited. Program funds can and do run out. Donors — including manufacturers — may stop making contributions, meaning exhausted funds may never be replaced.5
Funding program limits can take various forms:6
- Needs-based programs usually limit eligibility according to income, typically based on some multiple of Federal Poverty Guidelines. Coverage is often denied, especially for highly compensated employees.
- Therefore, alternative funding isn’t guaranteed. Individual members may find they don’t qualify for assistance or that funds have run out while their treatment is ongoing.
- Alternative funding vendors may not secure funding and then must work to carve drugs back into the original plan.
When funding stops or isn’t available, members need their employer to grant an exception to cover their medicine through the prescription benefit. The exception process creates additional administrative complexity — and costs — for plan sponsors. For example, exceptions may require time-consuming coordination among the alternative funding vendor, the plan sponsor and the PBM.7
Changing the pharmacy benefit to accommodate alternative funding programs can also alter the plan’s cost structure. This can affect pharmacy network rates, drug rebates, prior authorization approval rates and savings, costs associated with non-targeted medications, and short-term versus maintenance therapies.8
How alternative funding works
The cost savings from using charitable funds may seem attractive at first. But plan sponsors must realize their new vendor may not be able to secure funding or the funding may run out. They could end up paying more, not less.9
Below, we illustrate how a client’s costs might vary from the claimed alternative funding savings. The graph shows costs for an individual member granted $10,000 for a specialty drug through alternative funding. The middle line represents the normal PBM contract. Bars below that line show extra savings, and bars above the line show added costs.*
*Note: Figures are illustrative. Actual results will vary. Contact your Optum Rx representative for details.
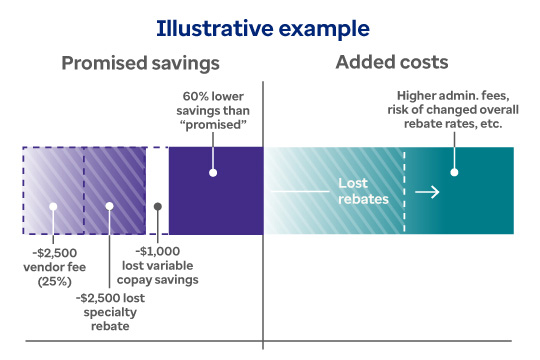
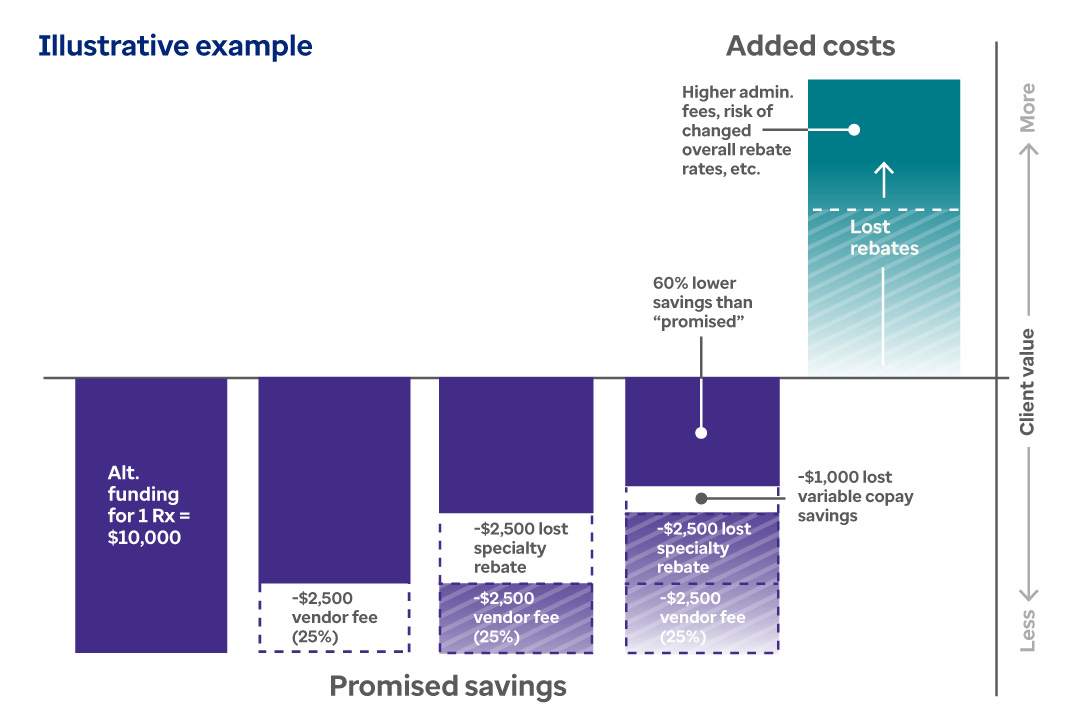
Bars below the center line indicate extra savings; bars above the line indicate added costs. Promised savings of $10,000 is shown below the center line for a specialty drug through alternative funding. The next three bars show decreasing saving amounts: $2,500 for vendor fees; $2,500 in lost rebates; $1,000 in lost variable copay savings. In total, savings are reduced by 60%. The last bar shows how costs can increase with higher administrative costs, changed rebate terms, etc., due to alternative funding arrangements.
Potential member disruption
Patient funding alternative programs can also affect the member’s experience. The process of having coverage denied, applying for aid, and waiting to see if funds are available takes time.
A member may go through the process only to find they’re ineligible for needs-based funding because they earn too much. Or, perhaps they are eligible, but all of the program’s funding has already been used.10
Clinical risk
Treatment delays can have very serious consequences. For example, when cancer treatments — including chemotherapy — are delayed even 1 month, patients have up to a 13% higher risk of death. That risk keeps rising the longer their treatment is delayed.11
When or if the patient must be transferred back to their original coverage, there’s another risk for delayed care. The transfer process takes time, posing a serious risk of a gap in therapy. And the patient may suddenly incur out-of-pocket costs they're not prepared for.
Finally, specialty patients often have many medical needs. For example, rheumatology patients commonly have 3 or more chronic conditions.12 These patients need careful management to coordinate care, prevent waste, and monitor drug dose, site selection, and medication adherence and response.
Clinical management programs are a core value provided by a full-service PBM like Optum Rx. Our systematic, end-to-end specialty drug management includes cost and clinical management from the point of prescribing to dispensing, through first use and throughout treatment. This strategy offers better value through holistic, coordinated care.
Ethical and legal considerations
Some alternative funding programs carry potentially harsh consequences for both plan sponsors and members. But consider the ethical issues:
- Charity funds and manufacturer assistance programs are intended for patients who don’t have insurance coverage. These funds play a vital role.
- Alternative funding vendors can charge payers up to 25% of the savings they achieve. But this means diverting critically needed funds away from uninsured patients.
- The inevitable result is less money for uninsured patients while the alternative funding vendors profit. It's an ethical dilemma that puts patient access to needed care at risk.
Ethical concerns can also become potential legal concerns as well.
Industry observers believe some funding alternatives could introduce discrimination risk into a client’s benefit structure. Self-insured plans could face ERISA and IRS compliance issues.13
Some alternative funding vendors will try to source needed drugs from a foreign market if they can’t secure funding through a patient assistance program.14 Foreign sourcing for prescription drugs is an intricate area of the law. Plan sponsors may want to seek additional guidance to avoid complications. Also, these international programs generally ship 90 days of high-cost specialty medication at a time, which increases the chance of waste.
Additionally, alternative funding vendors usually require individual members to sign a patient authorization form. The form certifies that they’re not enrolled in a health care program that pays for any part of their prescription drug costs.15
Consider nontraditional funding sources with caution
An online search for alternative funding programs typically presents them in a positive way — if they aren’t outright sales pitches.16 But some alternative funding schemes cause more problems than they’re worth. Anyone thinking about an alternative funding program should consider this option carefully.
For example, ask:
- What happens when the alternative funding ends or runs out?
- How will my plan afford these medications when they suddenly need to be funded again?
At Optum, we encourage longer-term and sustainable strategies over short-term solutions that can pose financial and regulatory risks. We strongly urge our clients to look past the short-term sales pitch and consider longer-term financial implications, compliance risk and ethics of alternative funding programs.
Contact your consultant or Optum representative to learn more about your options.
Related resources

Gene therapy: How to prepare for a growing pipeline

Specialty drug prices giving you sticker shock?

The dangers of polypharmacy
Sources
- AIS Health. Industry Experts Question Alternative Funding Companies That Carve Out Some Specialty Drugs, ‘Abuse’ Charities. Published September 1, 2022. Accessed September 7, 2022.
- Drug Channels. The Shady Business of Specialty Carve-Outs. Published August 2, 2022. Accessed August 2, 2022.
- AIS Health. Industry Experts Question Alternative Funding Companies That Carve Out Some Specialty Drugs, ‘Abuse’ Charities. Published September 1, 2022. Accessed September 7, 2022.
- Amwins Rx; Amwins Group Benefits, LLC. Stealth Targeted Patient Assistance Program (PAP). Accessed September 12, 2022.
- AIS Health. Industry Experts Question Alternative Funding Companies That Carve Out Some Specialty Drugs, ‘Abuse’ Charities. Published September 1, 2022. Accessed September 7, 2022.
- ibid.
- Rx Benefits. Excluding or Carving-Out Specialty Drugs: What Employers Need to Know. Accessed August 4, 2022.
- ibid.
- AIS Health. Industry Experts Question Alternative Funding Companies That Carve Out Some Specialty Drugs, ‘Abuse’ Charities. Published September 1, 2022. Accessed September 7, 2022.
- Rx Benefits. Understanding Alternative Funding for Specialty Medications. Accessed September 14, 2022.
- BMJ. Every month delayed in cancer treatment can raise risk of death by around 10%. Published April 11, 2020. Accessed September 14, 2022.
- AIS Health. Industry Experts Question Alternative Funding Companies That Carve Out Some Specialty Drugs, ‘Abuse’ Charities. Published September 1, 2022. Accessed September 7, 2022.
- Drug Channels. The Shady Business of Specialty Carve-Outs. Published August 2, 2022. Accessed August 2, 2022.
- Mercer. Prescription drug importation gets renewed attention. Published February 21, 2020. Accessed September 15, 2022.
- AIS Health. Industry Experts Question Alternative Funding Companies That Carve Out Some Specialty Drugs, ‘Abuse’ Charities. Published September 1, 2022. Accessed September 7, 2022.
- Forbes. How Alternative Funding Programs Can Ease the Cost Burden of Specialty Drugs. October 13, 2021. Accessed September 15, 2022.
