America's chronic shortage of health care workers is a major problem. The American Association of Medical Colleges (AAMC) forecasts a shortage of as many as 122,000 physicians by 20321 while U.S. News and World Report claims that the "growing shortage of health care workers is being called the nation's top patient safety concern."2 During the pandemic, a recent report revealed over 333,942 health care providers quit their jobs.3
This shortage has resulted in an estimated 30 million Americans living in medical deserts, meaning that they must travel more than 30 minutes to their nearest medical facility. Vermont, Alaska, Arkansas, Alabama and Maine have the largest populations dealing with this issue.4
These numbers highlight the supply-demand mismatch in the U.S. health care system. To address this, health care providers are looking to less traditional methods to reach patients through tools such as asynchronous virtual care. But often these solutions are not embedded into a holistic primary care solution.
There's also another issue that we all must be aware of: Providers are overworked and burned out, leading to increased strain on a workforce that is already stretched thin.
The Journal of the American Medical Association (JAMA) study showed that over the last 3 years, this emotional burnout has become a critical concern for providers. In 2019, nearly 32% reported feeling burned out. But after the pandemic, that number is now more than 49%.5
Long story short, the current health care system has fewer resources than ever and is struggling to provide care to an increasingly unhealthy and aging U.S. population. It's as if the health care system is like a traffic jam, trying to route volume for an 8-lane highway down to a single lane.
The impact of this shortage is far-reaching and widespread, causing serious issues not only for providers and their patients but for business owners as well. Those owners are concerned with the care that their workforce will get, as well as how this all affects their bottom line. Because after all, when their employees can't access care, they become unhealthier and – in the end – cost the employer more money.
As one employer said, "We're all over the country, including some remote parts. We want people to be able to get high-quality care without having to travel hundreds of miles to find a provider. I know sometimes that's necessary, but also they need a variety of providers who are easily accessible to them within the areas of the country in which they live."
Business owners may likely believe that these issues with the health care system will not be resolved anytime soon. To preserve the essential well-being of their workforce, many have taken on the pressure of trying to solve the problem themselves. A recent study has shown that 84% of employers feel very responsible for their employees' understanding of health care costs.6 Additionally, the Consolidated Appropriations Act, which passed in 2022, will raise the responsibilities of self-insured employers so they will have more interest in the quality and cost of the health services they offer.7
Even with an employer's traditional methods of addressing health care concerns — providing a high-quality health plan offering, robust benefits and an expansive provider network — issues like a lack of access and a lack of connectivity across care sites won't be going away. That's why most patients wait an average of 26 days to see a primary care provider (PCP)8 and why we see, in a 2021 McKinsey study, that 65% of full-time employees of large U.S. employers report having experienced at least one unmet basic health need.9
In the past, employers have also tried to solve these issues by bundling point solutions together. But these solutions only ended up frustrating employees because each solution is in a silo, only serving one health care need. As none of these separate solutions share information, HR departments struggle with making all of their disparate services play nicely together. Plus, if a plan is difficult for an HR team to navigate, it’s most certainly going to confuse employees. That's one of the reasons why 79% of consumers want a single point of contact for their care.10
One employer stated, "We offer all these programs and services to our members, and they're great assets for members to have access to. But at the end of the day, if the members don't use them then all you're doing is paying some type of administrative fee or some type of fee associated with it. You're not getting the utilization that you really need."
So what can we do about it?
This unmet need creates an opportunity to innovate. Employers can improve health outcomes through careful plan design11 inclusive of workplace health services and a full-service virtual primary and behavioral health service. Optum is uniquely positioned to respond with these services because of their superior access, broad options of virtual to in-person care sites, deep health care knowledge, quality of care and the ability to integrate with other member-sponsored health benefits. Optum offers easier access to care through flexible options to engage with health care services virtually or in-person in a meaningful way. That way, the services all work together to drive value for the employer, and — most importantly — deliver better, more holistic care for employees.
In short, Optum is creating truly convenient, comprehensive and value-based care by giving employees better options to access care on their terms. It's not just workplace wellness. It's about fundamentally redesigning how people think about accessing and engaging with care.
An on-site workplace solution can create a health care "home" for hybrid workforces, giving them a place that is available during the workday and a virtual care wraparound for their care needs during off-hours as well as a connection to expert health care navigators. With a focus on empowering and educating patients, the on-site care team helps patients develop strategies to make lasting lifestyle adjustments and bolster overall wellness, disease management and recovery from illnesses, all with the goal of equality of care across the full employee population.
One of the reasons Optum has put this solution together is because we know health care is dynamic and requires a multi-pronged approach to meet people where they are along their health journey. All of the multiple services that employees need to stay healthy make up our comprehensive employer health solution, and to make it all work, they must be connected in a meaningful way.
What do we mean by meaningful? We feel that patients should expect more, including easy access to the care that they need, a holistic view of their health so they know how to manage it between provider visits, and connection to employer-sponsored programs and guided chronic condition management to make sure that they’re using their benefits package to its fullest potential.
This model of care becomes something like air traffic control. Controllers direct flight paths for thousands of planes, helping them land on time and keep everybody safe. Our goal is to create a similar experience for our patients by providing care when and where patients need it and guiding them to next-level care when necessary — and before the moment of opportunity has passed.
Here’s an example of how it works:
Here’s an example of how it works:
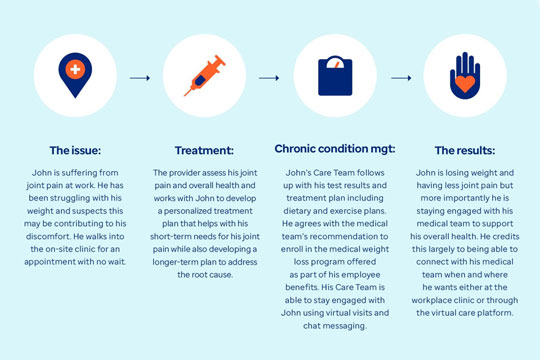
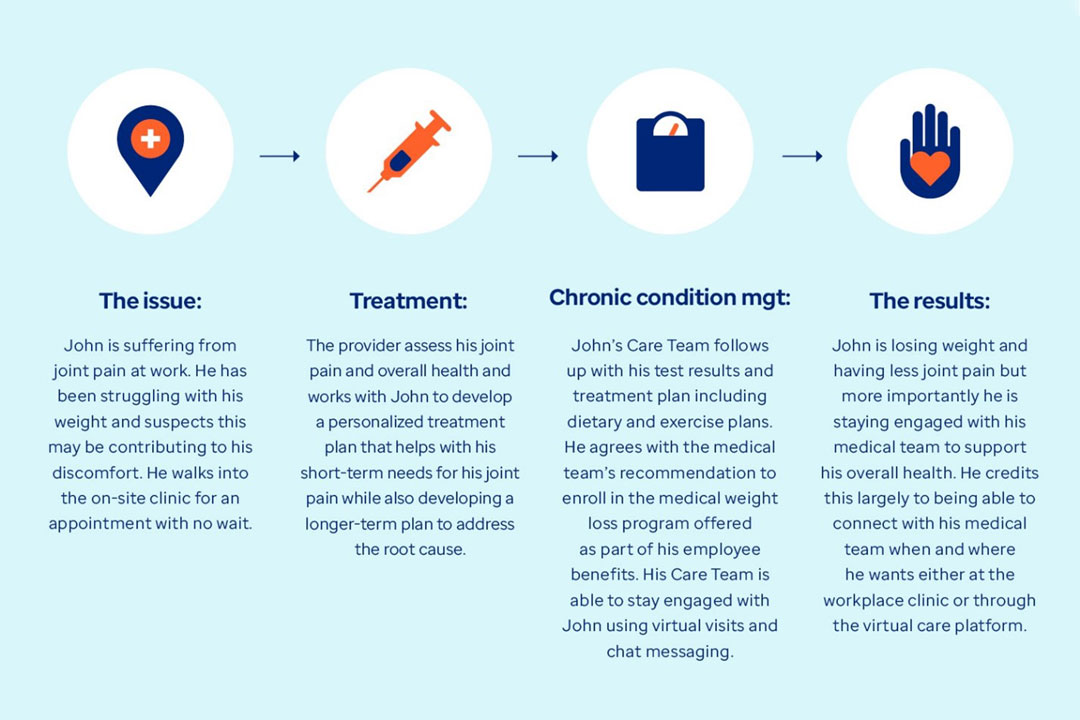
The issue: John is suffering from joint pain at work. He has been struggling with his weight and suspects this may be contributing to his discomfort. He walks into the on-site clinic for an appointment with no wait.
Treatment: The provider assesses his joint pain and overall health and works with John to develop a personalized treatment plan that helps with his short-term needs for his joint pain while also developing a longer-term plan to address the root cause.
Chronic condition management: John's Care Team follows up with his test results and treatment plan including dietary and exercise plans. He agrees with the medical team's recommendation to enroll in the medical weight-loss program offered as part of his employee benefits. His Care Team is able to stay engaged with John using virtual visits and chat messaging.
The results: John is losing weight and having less joint pain, but more importantly, he is staying engaged with his medical team to support his overall health. He credits this largely to being able to connect with his medical team when and where he wants — either at the workplace clinic or through the virtual care platform.
Remember that massive traffic jam?
Our goal is to create an off-ramp before things get that rough. Quickly addressing employee health needs reduces strain on our already overloaded health care system and lightens the burden on business owners trying to keep up productivity and retain their workforces.
How will we do that? When employees have a convenient place to seek care, they can stay healthier, avoid long waits for a PCP appointment and seek care in the right setting, rather than using the emergency room for regular health care needs. Additionally, our health coaching and chronic condition management focus on engaging the workforce early to get better outcomes and reduce health care expenditures. By using both physical and digital tools, the employee experience improves, as does that of the medical team. This model brings the convenience people are looking for while helping the health care system work more efficiently to help address workforce challenges.
As an example, we provided one of our clients with 7 on-site clinics to address the health needs of 21,000 employees and their dependents. We offered primary care, population health, chronic condition management, occupational health and telemedicine services, and used our advanced analytics to identify high-risk patients who would benefit most from proactive outreach.
The results
The results
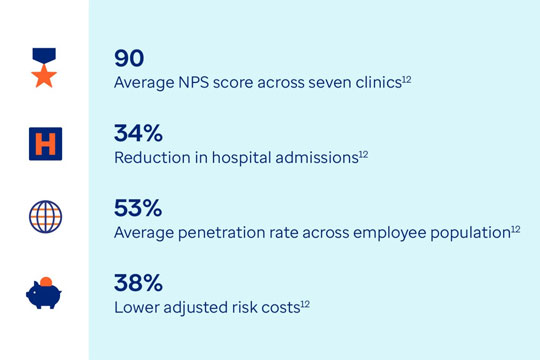
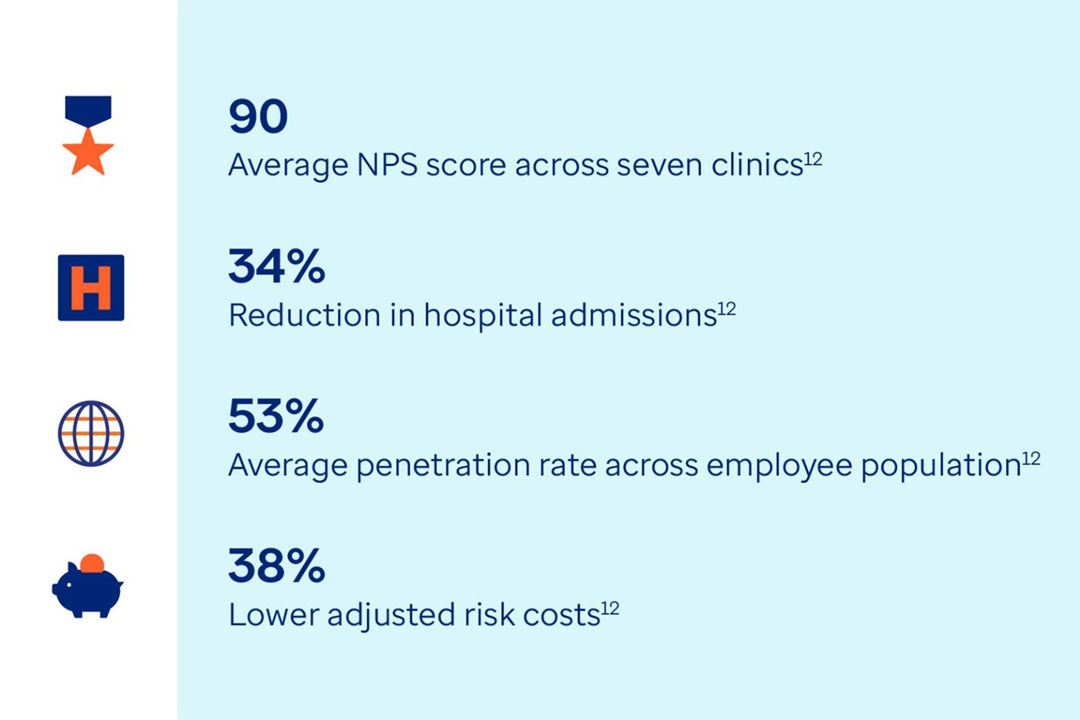
90: Average NPS score across seven clinics12
34%: Reduction in hospital admissions12
53%: Average penetration rate across employee population12
38%: Lower adjusted risk costs12
- Association of American Medical Colleges: New Findings Confirm Predictions on Physician Shortage. Accessed November 4, 2022.
- U.S. News and World Report: Staff Shortages Choking U.S. Health Care System. Accessed November 4, 2022.
- Modern Healthcare: Physicians left their jobs by the hundreds of thousands in 2021: report. Accessed January 17, 2023.
- Washington Examiner: Medical deserts strand millions without access to life-saving healthcare. August 9, 2022. Accessed December 1, 2022.
- Journal of the American Medical Association: Emotional Exhaustion Among US Health Care Workers Before and During the COVID-19 Pandemic, 2019-2021. Accessed November 4, 2022.
- SHRM: Employers Are Feeling Employees' Financial Pain, Enhancing Benefits. October 14, 2022. Accessed October 17, 2022.
- Fierce Healthcare: Consolidated Appropriations Act shifts more power, responsibility to employers next year. Accessed January 17, 2023.
- Merritt Hawkins: PCP wait times report based on the 15 largest metropolitan areas in the United States. Accessed November 4, 2022.
- McKinsey & Company: Income alone may be insufficient: How employers can help advance health equity in the workplace. Accessed January 17, 2023.
- Huron Consulting Group: Healthcare Consumer Market Report. Accessed December 1, 2022.
- Harvard Business Review: Employers Can Do More to Advance Health Equity. Accessed January 17, 2023.
- Optum: ROI Summary of Optum On-Site Clinic Utilization, 2019. Accessed December 1, 2022.
Wait time subject to patient volume and provider availability. Prescriptions available only where medically necessary in the sole discretion of provider. Other restrictions may apply.
