Cross Optum programs turn evidence into action
In this fragmented healthcare landscape, life sciences organizations are faced with the challenge of how to connect the pieces. They’re asking how to:
- Improve efficiency of timely diagnosis
- Test new processes that could improve clinical decision-making and therapy adherence
- Discover effective ways to improve guidelines for directed therapy and evidence-based medicine
- Understand patient and provider behavior in the real world
- Educate patients on therapy options and the benefits of staying on track with their treatment
Small changes can make a big difference. The Cross Optum team works with life sciences companies and the larger UnitedHealth Group® enterprise to identify unmet needs, design and pilot engagement programs, and evaluate outcomes.
Connecting parts of the healthcare ecosystem
Our team uses implementation science to generate evidence that serves as a catalyst to improve the future of health care.

Key benefits
Clinical programs and process improvements to existing interactions help foster adoption across stakeholders. We focus on the following:
Disease awareness and prevention
Identify at-risk individuals and help resolve healthcare gaps.
Guideline-directed care
Improve quality and consistency of patient care across the healthcare ecosystem.
Treatment, intensification and adherence
Collaborate to increase adherence and improve outcomes.
Case study
Lowering cardiovascular disease risk
An innovative program involving patient awareness and provider outreach helps improve patient use of lipid-lowering therapies.
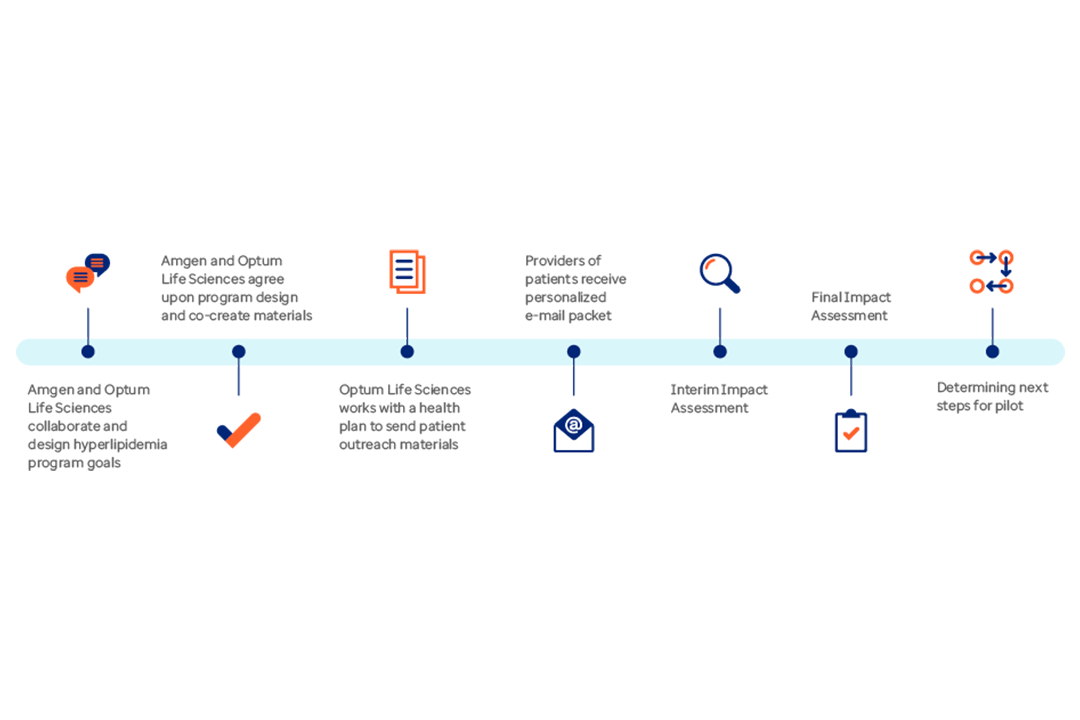

Build evidence to reach and treat the right populations
Optum designed a program to introduce an assessment tool and prepare clinicians with training and a guide to aid diagnosis and treatment.
Related healthcare insights
Article
An innovative program involving patient awareness and provider outreach improves patient use of lipid-lowering therapies.
Article
Ask your life sciences stakeholders what they need early on. Consider these top questions that patients, providers, payers and regulators are looking to answer.
White paper
Proving the impact on clinical outcomes as well as costs.